Globus Pharyngeus
Definition.
Swallowing is a complicated sequence of both voluntary and reflex movements, which needs your brain to coordinate many muscles and nerves.
Dysphagia is the medical term for a sensation of difficulty or abnormality of swallowing. It can happen rapidly, or slowly and has many causes.
Globus Pharyngeus: The term “globus” is derived from the Latin meaning “ball”. It is defined as at least 12 weeks, in the preceding 6 months of:
- persistent or intermittent, non-painful sensation of a lump or foreign body in the throat….
- in the absence of dysphagia,
- in the absence of oesophageal pathology.
Globus is extremely common, affecting up to 46% of healthy middle-aged people. The condition accounts for around 4% of ENT referrals worldwide.
Causes:
A number of underlying mechanisms for globus have been proposed including:
- Gastro-oesophageal reflux
- Cricopharyngeal spasm
- Pharyngeal and Oesophageal dysmotility
- Pharyngeal and Oesophageal hypersensitivity..
But the underlying causes remains unclear. Gastro-oesophageal reflux remains the most favoured cause for globus. For example, from studies, a person with reflux symptoms has ~ 2 times the odds of experiencing globus, compared with a person without reflux symptoms. Oesophageal hypersensitivty in patients with globus hasalso been demonstrated in a number of studies. Life stress might be a co-factor in the genesis or exacerbation of globus symptoms.
Patients often worry that the symptom of globus may be the first sign of an upper aero-digestive tract cancer. However, studies have shown that it is exceedingly rare for globus to be the sole presenting symptom, and cancer is usually accompanied by pain, dysphagia, or hoarseness.
A number of upper pharyngo-oesophageal conditions have been reported in globus sufferers, such as hiatus hernia, cervical osteophytes, cricopharyngeal bar, cervical web, and heterotopic gastric mucosa (stomach lining tissue found in the upper oesophagus). However, these conditions are found no more commonly in globus sufferers than in the general population.
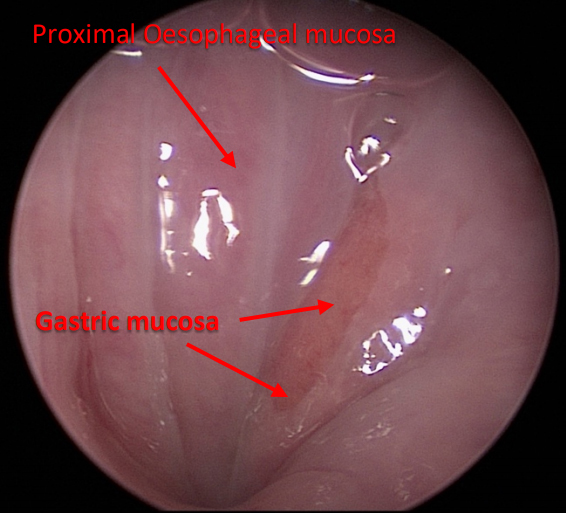
Fig. 1 – heterotopic gastric mucosa
Diagnosis:
The diagnosis of pure globus is generally achieved with a careful history, physical examination and digital naso-laryngopharyngoscopyalone. Rarely, in the absence of additional symptoms or findings, are further investigations required.
If indicated, an instrumental swallowing evaluation such as Flexible Endoscopic Evaluation of Swallowing and/or a Videofluoroscopy Swallowing Study (x-ray) may be utilised.
Additional tests are rarely required for pure globus, but may include Trans-nasal Oesophagoscopy, barium swallow, and High Resolution Oesophageal Manometry to exclude any muscular cause for your symptoms may also be performed. A validated questionnaire, called a patient-related outcome measure, is often completed initially, and repeated later on to measure your progress. E.g. Eat-10 or SWAL-QOL.
Management:
Once you have had a complete swallowing evaluation, the swallowing specialists can recommend ways to improve your ability to eat and drink depending on the specific problems found:
- Conservative Treatment:
- Explanation and reassurance: Given the benign nature of the condition, the likelihood of persistent symptoms long-term, and the absence of evidence for the effectiveness of treatments, the mainstay of treatment rests with explanation and reassurance.
- Proton Pump Inhibitors: There are grounds for a trial of a PPI, especially where typical reflux symptoms are present.
- Coagluation ablation of cervical oesophageal inlet patch: One small study has demonstrated, that, ablation of cervical oesophagela inlet patch mucosa, when present, can alleviate globus.
- Behavioural and Psychotropic Therapies:
- There is some anecdotal evidence of symptomatic benefit with the use of tricyclic antidepressants.
Initial recommendations:
- Take your time when eating and drinking
- Take smaller mouthfuls and chew well
- Alternate liquids with solids to clear residue.
- Ask your GP or physician today whether you need a swallowing evaluation.
- See your GP urgently if you are coughing and choking after swallowing, have a fever, or a productive cough.
