Definition.
Swallowing is a complicated sequence of both voluntary and reflex movements, which needs your brain to coordinate many muscles and nerves.
Dysphagia is the medical term for a sensation of difficulty or abnormality of swallowing. It can happen rapidly, or slowly and has many causes.
Vocal Cord Paralysis/paresis is the term used when one or both vocal cords no longer move completely to close to protect the airway, cough or voice. It happens when the nerves to your vocal cords (larynx) are disrupted/damaged. These nerves can be damage anywhere along their course from the brain to their insertion into the vocal cords and surrounding muscles.
Causes:
The Vagus nerve and its branches, (recurrent and superior laryngeal nerves) control the movements and sensation to the voice box. Neurological injury can occur anywhere from the brainstem to the chest. It can cause paralysis of the swallowing muscles, poor sensation and reflexes in your throat, and/or impaired closure of the upper airway during the swallowing process.
Some common causes are:
- Viruses and infections.
- Strokes
- Tumours of the head, neck, chest and oesophagus.
- Direct Injury (cutting, crushing, stretching, etc) to the nerves during surgery – e.g. Cervical Spine Surgery, Thyroid Surgery, Carotid surgery.
- Neurodegenerative diseases.
- Auto-immune diseases.
- Trauma to the neck or chest.
Symptoms:
These conditions affect the ability to swallow fluids, saliva and often solids, as well as voice quality, cough strength, and breathing.
The degree of difficulty can depend on:
- How high up the nerve the injury occurred – generally the higher in the neck or closer to the brain, the more severe the swallowing difficulty.
- Time elapsed, and therefore degree of wasting/weakness, or recovery, since injury.
- Whether the throat (pharynx) is affected or only the voice box.
- Degree of sensory injury to the pharynx and voice box.
- Presence and severity of any additional neurological injury, or throat injury.
The swallowing problem needs regular monitoring to ensure that food and fluid can be taken safely and that nutrition is maintained.
Symptoms you may experience include:
- Breathy, weak voice.
- Weak, ineffective cough.
- Food or liquids getting ‘stuck’ in your throat.
- Coughing or choking while swallowing.
- A wet ‘gurgly’ sounding voice.
- Taking longer to finish a meal.
- Loss of weight.
- Recurrent pneumonia.
Diagnosis:
The presence of a vocal cord paralysis/paresis is diagnosed via nasendoscopy by an Otolaryngologist (ENT Surgeon). Brain imaging such as MRI, and Neck/chest imaging such as CT will be ordered to visualise the entire course of the vagus and recurrent laryngeal nerves. These scans will also provide important information about the area(s) of the nerve that have been affected, and further inform the impact it may have on your swallowing, voice and airway function.
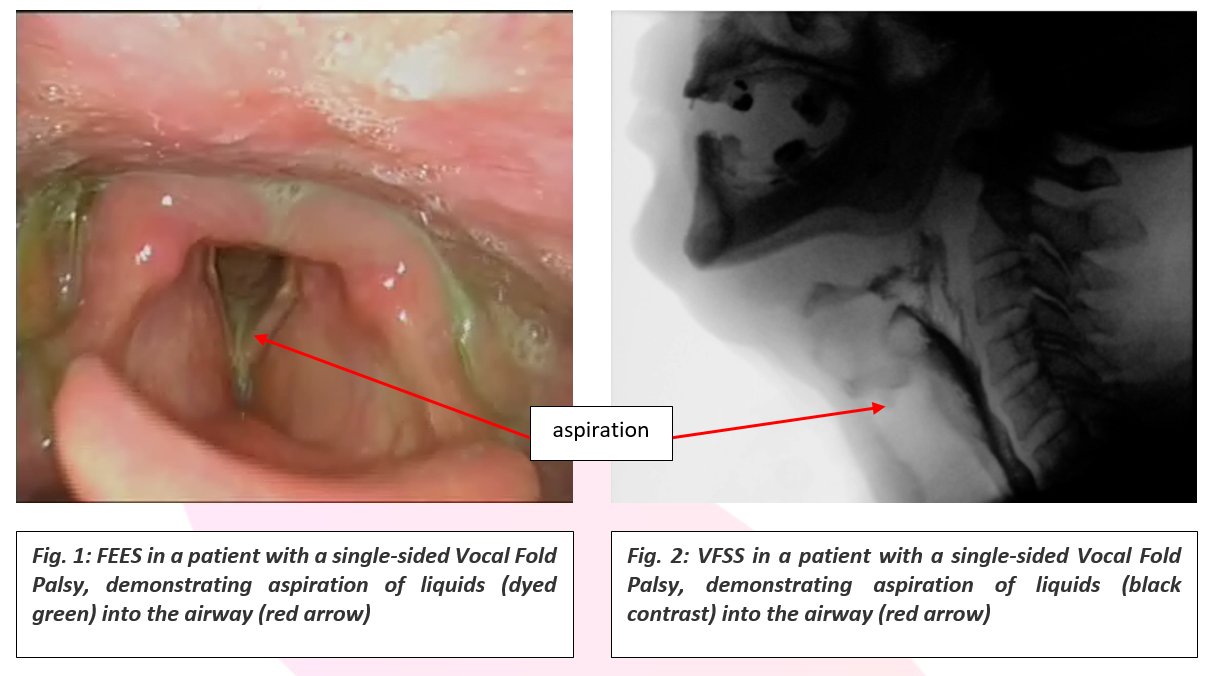
The diagnosis of dysphagia involves a thorough case history, clinical examination of the muscles and nerves required for swallowing, digital nasendoscopy of the upper airway and pharynx, and an instrumental swallowing evaluation such as Flexible Endoscopic Evaluation of Swallowing (FEES) and/or a Videofluoroscopy Swallowing Study (x-ray) (VFSS).
Additional tests may be required such as a standard barium swallow, and High Resolution Pharyngeal Manometry to exclude any muscular cause for your symptoms. A validated questionnaire, called a patient-related outcome measure, is often completed initially, and repeated later on to measure your progress. E.g. Eat-10 or SWAL-QOL.
Management:
Your ENT surgeon will advise the best acute and long-term treatment for the vocal fold paralysis/paresis and its underlying cause.
Once you have had a complete swallowing evaluation, the swallowing specialists can recommend ways to improve your ability to eat and drink depending on the specific problems found:
- Specific Treatments:
- If you have persistent vocal cord weakness, this may be able to be treated with a procedure to improve closure of your vocal cord – g. vocal cord filler injection, or silicon/gore-tex® medialisation procedure.
- Botulinum Toxin may occasionally be injected into tight swallowing muscles.
- Swallowing Modifications:
- Exercise to promote muscle strength and co-ordination.
- Strategies to improve swallowing safety – g. tucking chin down, turning head to side.
- Dietary Modifications:
- Thickening drinks with specialised products to reduce the likelihood of it going down the wrong way (into your airway).
- Softening your food to make it easier to swallow.
Initial recommendations:
- Take your time when eating and drinking.
- Avoid distractions such as television or other people when eating / drinking.
- Use a teaspoon to take smaller mouthfuls.
- Eat smaller meals more often if swallowing is tiring.
- Ask your GP or physician today whether you need a swallowing evaluation.
- See your GP urgently if you are coughing and choking after swallowing, have a fever, or a productive cough
