Swallowing information for Zenker’s Diverticulum (Pharyngeal Pouch)
Definition:
Swallowing is a complicated sequence of both voluntary and reflex movements, which needs your brain to coordinate many muscles and nerves.
Dysphagia is the medical term for a sensation of difficulty or abnormality of swallowing. It can happen rapidly, or slowly and has many causes.
The pharynx is that part of the upper aero-digestive tract, that lies between the mouth, and the oesophagus. It is has a muscular wall, and outer lining connective tissue.
Pharyngeal Diverticula are outpouchings of the wall of the pharynx. They can lie in the midline, behind the pharynx, of out to one side. They can lie above the Cricopharyngeal muscle (sphincter-like muscle at the upper end of the oesophagus) or below it.
A Zenker’s Diverticulum herniates out backwards as a pouch from the pharynx, above the Cricopharyngeal muscle.
It is a fairly uncommon condition, occurring most commonly in men in their 70s and 80s, with an incidence of 0.01% to 0.11%.
Causes:
There is some controversy over the cause of a Zenker’s Diverticulum, but broadly speaking it is the consequence of 2 factors. First, in all of us, there is a natural area of weakness in the back-wall of the pharynx, lying just above the CP muscle, and just below the Inferior constrictor muscles.
In patients with a Zenker’s, there is a loss of muscle compliance in the area of the CP muscle due to scarring and degeneration, and this causes elevated pressures over the area of weakness as food travels down. Over time, this elevated pressure causes an outpouching at this area of weakness until a Zenker’s Diverticulum forms.
Diagnosis:
The diagnosis of dysphagia involves a thorough case history, clinical examination of the muscles and nerves required for swallowing, digital nasendoscopy of the upper airway and pharynx, and an instrumental swallowing evaluation such as Flexible Endoscopic Evaluation of Swallowing (FEES) and/or a Videofluoroscopy Swallowing Study (VFSS).
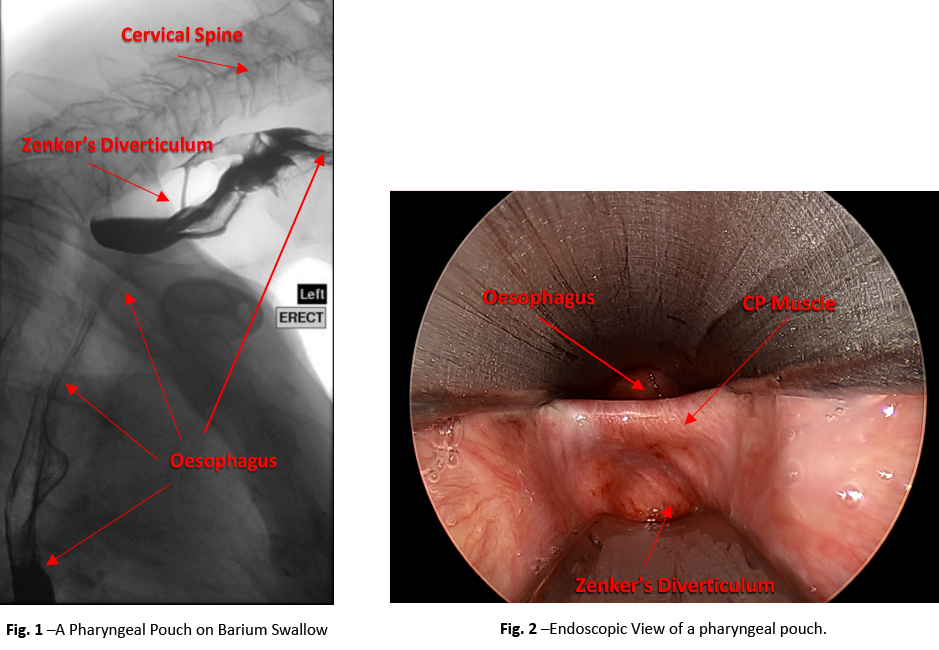
Additional tests may be required such as a standard barium swallow (SEE Fig. 1), High Resolution Pharyngeal and Oesophageal Manometry, , 24 hr pH/Impedance monitoring and/or oral salivary pepsin testing (Peptest). A validated questionnaire, called a patient-related outcome measure, is often completed initially, and repeated later on to measure your progress. E.g. Eat-10 or SWAL-QOL.
Symptoms you might experience in the diagnosis of Zenker’s Diverticulum are generally due to a combination of food/residue accumulating in the pouch, and inelasticity of the CP muscle just above the pouch. They include:
- a sensation of a lump in the throat
- difficulty swallowing solids +/- liquids
- coughing or choking after swallowing
- regurgitation of undigested food, (very common – 80% of patients)
- audible gurgling during swallowing
- bad breath
- Weight loss
If you can’t swallow correctly then food and drink may be getting into your airway and lungs. This is called aspiration. If this happens it can lead to infections and pneumonia, which can be very serious. It is important that any changes to your swallowing are identified early, to avoid this happening.
Pouch related complications may occur, the most important being the development of a Squamous Carcinoma in the pouch. This is quite rare (0.4-1.5%), but any sudden worsening of your symptoms (e.g. pain, coughing up blood) needs to be reported to your health professional.
Management:
Once you have had a complete swallowing evaluation, the swallowing specialists can recommend ways to improve your ability to eat and drink depending on the specific problems found. There are a variety of different treatment options depending on the cause/s and severity of presentation.
- Procedural/ Surgical Treatments:
- Endoscopic Zenker’s Diverticulolostomy: This approach involves dividing the wall between the pouch and the oesophagus, creating a common pouch, which also thus divides the scarred and thickened CP muscle. (SEE Fig. 2). The division is achieved using a combination cutting/ sealing device such as a Stapler, ENSEAL® or Liga-Sure® (SEE Fig. 3), or sometimes a Laser. There are no incisions in the neck, the operation is fairly rapid, and the complication rate is low, (approximately 5.5%). Patients are often eating and drinking the following day.
- Open Zenker’s Diverticulotomy with Cricopharyngeal myotomy: This approach involves excising the pouch from the oesophagus and oversewing the stump. The Cricopharyngeal muscle is also incised at the same time to minimise the chance of recurrence. The advantage of this approach is that is can be employed on any size of pouch, and it eliminates the very small possibility of cancer in the residual pouch wall (as in an endoscopic approach). However, the open approach has a longer operating time, has a higher complication rate (approximately 11.8%), and a delayed return to oral intake, and increased hospital stay.
- Other Surgical Approaches:
- Endoscopic: in rare cases, a flexible scope assisted endoscopic stapling is performed due to difficult access, but has high recurrence rates.
- Open: In some cases, the pouch is ‘hitched’ upwards to pre-vertebral tissue rather than being excised. This is particularly beneficial when the sac is very large, or healing is a concern.
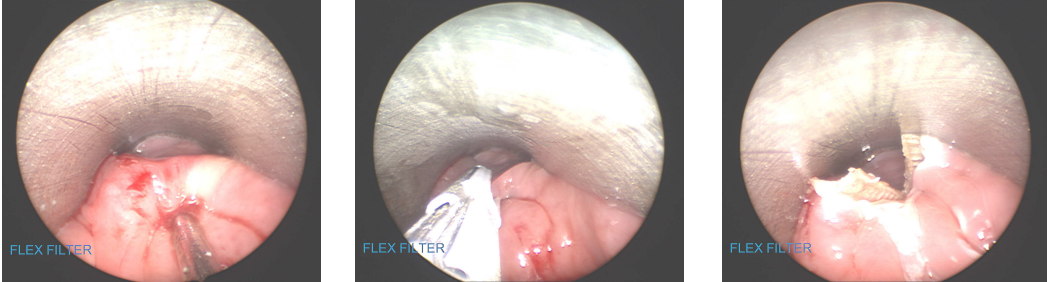
Fig. 3-5 – Endoscopic Zenker’s Diverticulostomy using ENSEAL® Device.
- Swallowing Modifications:
- General strategies to improve swallowing safety such as tucking chin down, turning head to side, may be employed.
- Safe swallowing strategies such as eating slowly or taking smaller mouthfuls, may also be advised.
- Dietary Modifications
- Softening your food to make it easier to chew and swallow.
Initial recommendations:
- Take your time when eating and drinking
- Avoid distractions such as television and other people
- Use a teaspoon to take smaller mouthfuls
- Eat smaller meals more often if swallowing is tiring.
- Ask your GP or physician today whether you need a swallowing evaluation.
- See your GP urgently if you are coughing and choking after swallowing, have a fever, or a productive cough.
