Swallowing Problems after Cervical Spine Surgery
Definition:
- Swallowing is a complicated sequence of both voluntary and reflex movements, which needs your brain to coordinate many muscles and nerves.
- Dysphagia is the medical term for a sensation of difficulty or abnormality of swallowing. It can happen rapidly, or slowly and has many causes.
- Anterior cervical discectomy and fusion (ACDF) is a type of neck surgery that involves removing a damaged intervertebral disc, and stabilising the cervical spine to relieve spinal cord pressure and improve corresponding pain, weakness, numbness, and tingling.
The ACDF surgery has 2 parts: (SEE Fig. 1)
- Anterior cervical discectomy. The spine is approached through the anterior (front) or posterior (behind) aspect of the neck. The disc is then removed from between two or more vertebral bones. To reach this area, the surgeon needs to retract and compress a number of neck structures (muscles, nerves, pharynx/oesophagus), and also avoid damaging these same structures
- Fusion: A cervical fusion is done at the same time as the discectomy operation in order to stabilize the cervical spine. A fusion involves placing bone graft and/or implants where the disc originally was in order to provide stability and strength to the area, and stabilising the neck with screws.
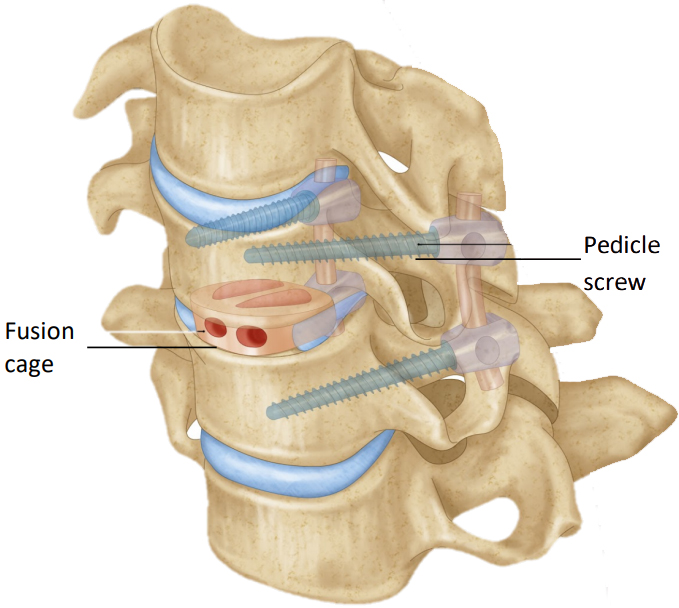
Fig. 1 –Anterior Cervical Discectomy & Fusion
Dysphagia is one of the most common complications following ACDF surgery. Most ACDF patients fully recover their ability to swallow within a few days after surgery. However, sometimes, the dysphagia lasts for weeks, months, or even longer. Studies estimate that about 10-30% of ACDF patients have some degree of swallowing difficulty for up to 2 years after surgery. There is arare risk that their dysphagia will be permanent
Causes:
The throat (pharynx), voice box (larynx) and food pipe (oesophagus) lies directly in front of the spine and needs to be mobilized and retracted during surgery. This can cause stretching, dislodgement or damage of the nerves and muscles required for swallowing. In addition, there have been reports of the fusion hardware obstructing the proper movement of the structures involved in swallowing. Sometimes post-surgical inflammation, infection, and scarring can also contribute to dysphagia.
If you can’t swallow correctly then food and drink may be getting into your airway and lungs. This is called aspiration. If this happens it can lead to infections and pneumonia, which can be very serious. It is important that any changes to your swallowing are identified early, to avoid this happening.
Diagnosis:
Your spinal surgeon will be familiar with these risks and monitor you after your surgery for any symptoms of swallowing or voice problems. If your problems persist, he/she is likely to refer you for further evaluation by swallowing specialists.
The diagnosis of dysphagia involves a thorough case history, clinical examination of the muscles and nerves required for swallowing, digital nasendoscopy of the upper airway and pharynx, and an instrumental swallowing evaluation such as Flexible Endoscopic Evaluation of Swallowing (FEES) and/or a Videofluoroscopy Swallowing Study (VFSS)
Additional tests may be requires such as a standard barium swallow and/or video-stroboscopy. A validated questionnaire, called a patient-related outcome measure (PROM), is often completed initially, and repeated later on to measure your progress –e.g. EAT-10 or SWAL-QOL.
Symptoms you might experience include:
- Weak cough and voice
- Foods or liquids getting stuck in your throat
- Coughing or choking while swallowing.
- A wet ‘gurgly’ sounding voice.
- A feeling of a ‘lump’ in your throat.
If you can’t swallow adequately, then food and drink may be getting into your airway and lungs. This is called aspiration. If this happens it can lead to infections and pneumonia, which can be very serious. It is important that any changes to your swallowing are identified early, to avoid this happening.
Management:
Once you have had a complete swallowing evaluation, the swallowing specialists can recommend ways to improve your ability to eat and drink depending on the specific problems found:
- Specific Treatments:
- If you have a focal muscular weakness of a vocal fold, this may be able to be treated with a procedure to improve closure of your vocal folds – e.g. vocal cord medialisation injection or implant.
- Exercises to improve muscle strength.
- Rarely, would parts of the fusion hardware require removal or revision due to post-operative dysphagia.
- Swallowing Modifications:
- Strategies to improve swallowing safety. E.g. effortful swallow, turning head to side whilst swallowing
- Safe swallowing strategies such as eating slowly or taking smaller mouthfuls.
- Dietary Modifications
- Softening your food to make it easier to chew and swallow.
- Thickening drinks with special powders to make them easier to swallow.
Initial recommendations:
- Take your time when eating and drinking
- Avoid distractions such as television and other people
- Use a teaspoon to take smaller mouthfuls
- Eat smaller meals more often if swallowing is tiring.
- Ask your GP or physician today whether you need a swallowing evaluation.
- See your GP urgently if you are coughing and choking after swallowing, have a fever, or a productive cough.
